
Have you ever worried about loosing weight? If yes, then you are not alone.
Weight is such a constant worry that almost half of the US population is trying to loose weight at a given time, according to data from Centers for Disease Control and Prevention (CDC).
That also explains the growing popularity of GLP-1 drugs such as Ozempic and Wegovy.
Despite all the efforts, a 2015-16 CDC report says almost 40 percent adults and 20 percent teenagers were obese. And these numbers are growing.
By definition, obesity is defined as body-mass index (BMI) above 30. BMI is calculated as weight (in kg) divided by square of height (in meters).
Another group, with BMI between 25 and 30 falls under the category of overweight. That’s slightly above the healthy range of 18 to 25.
Taken together, almost 70% of the US population is either overweight or obese (1). Globally, 39% of adults and 18% of youth were overweight or obese in 2016, the World Health Organization (WHO) reports (2).

MORE FROM OUR HEALTH BLOGS
Genetic Testing and Disease Inheritability – role of genetics on health.
Inflammation Biomarkers and Heart Failure - key biomarkers as risk factors in heart failures.
APoE, Alzheimer's, Dementia and CVD - the complex role of APoE gene.
Food Sensitivity and More – allergy, intolerance, and celiac disease.
Cortisol Risk Factors – the key risk factors to consider.
Obesity is a well known risk factor in heart disease and heart failure (3). According to a Framingham Heart Study, published in the prestigious New England Journal of Medicine publication (3), almost 11% men and 14% women had a heart failure that was attributable to obesity alone.
In this article, we will discuss BMI, its definition, and impact of being obese or overweight on heart health.

The above chart from CDC shows the growing trend of obesity and overweight population. It reflects the huge impact of BMI on public health, especially for heart disease and deaths from heart failure.
Recently, the Global BMI Mortality Collaboration, from University of Cambridge, UK, reviewed 239 studies of over 10 million people across North America, Asia, Australia and New Zealand (4). They found BMI has a strong impact on the overall health and called for strategies to combat this rapid rise in weight gain across the world.
Body-mass index (BMI) is a measure of body fat, calculated as the relative weight for a given height. Mathematically, it is weight in kg divided by square of height in meters (One needs to multiply by 703 when values are in lbs and square inches). Several online calculators are available to quickly assess BMI values and understand what the numbers mean. A value between 18 and 25 is healthy.
BMI is a popular metric because both height and weight are measurable, easily and accurately without any expensive tools. In reality, BMI is not a perfect indicator of body fat or obesity but rather a measure of relative heaviness.
The reliable measurement and reasonably well association to obesity and disease in larger groups makes BMI a widely popular indicator of population health. After a certain age height remains constant, therefore weight is a bigger contributor to BMI for monitoring health.
Typically, BMI increases with age. In men, it peaks around the age of 50 years and remains relatively constant, although women may see weight gain until in their 70s (5).
Blood relatives tend to have a narrow distribution of BMI, suggesting a strong genetic component (6). However, changes in BMI over a period of time is more due to the relative age instead of family history.
Smoking is closely associated with lower BMI, regardless of age (5), although smoking itself is an independent risk factor for coronary heart disease (CHD) and cardiovascular disease (CVD), both are associated with death from heart failure.
If the calories we consume do not fully burn-off , they deposit as excess fat. These extra calories then convert into triglycerides (TG) and deposit as fat (7).
This is the same fat we routinely consumer from fatty foods, and appears as triglyceride in a regular blood test. You might have to fast 8-12 hours before the test. That’s because TG levels in blood rise after a meal and return to baseline after few hours. This baseline depends on BMI and impacts the insulin release from pancreas.
Once we consume the food, conversion from glucose into fatty acids happens in liver. Insulin is the key molecule in this conversion. Over a period of time, resistance might develop when the extra calories require additional insulin production. That is why 70-80% of diabetes cases occur in those with excess weight (7).
Despite easy availability of fast food today, no consistent correlation between BMI and geographical access to fast food has been found in a study spanning over 30-year (8).
There was a weak correlation for women, showing every increase in 1-km distance from a fast-food restaurant, an average women had about 1 lbs lower weight (8). No such correlation was found among men.
Genetics play a major role in weight gain and management (9, 110), however, diet composition has an important role (11) to maintain it. CDC has several good recommendations on the strategies for maintaining a healthy weight.
Increase in weight can reflect in BMI, waist circumference/size, waist-to-hip ratio or fat around the neck. In fact, each of these factors independently correlate to certain risks.
Waist circumference and waist-to-hip ratio have been shown as better predictors of risks of death from heart disease and cardiovascular disease (12). High waist-to-hip ratio–in combination with hypertension (above 140/90 mmHg)–has been shown to affect cognitive decline (13).
Extra fat around waist has been associated with smaller brains in middle-aged men and women (14).
In general, waist circumference seems to be a better predictor of health than waist-to-hip ratio (32). In a study of over 50,000 men, waist circumference directly associated with the risk of diabetes in the top 20% cases. The number was about 5% for waist-to-hip ratio (15).
In another study, fat around the neck has been shown to increase the risk of diabetes (16).
Being overweight (BMI 25 to 30) specifically increases the risk of hypertension, chest pain (angina) and heart disease (CHD) although risk for high cholesterol, diabetes are more correlated to being obese (17). Being overweight especially increases the risk of heart disease, CVD and stroke in men, although women also show strong correlation to high rates of hypertension and chest pain.
Obesity is a risk factor of heart disease because it strongly correlates to high cholesterol, blood pressure and blood glucose, which also increase the risk diabetes, cancer, and early death (18). This is true for BMI as well as waist size (19). However, without regular monitoring over years, this relationship can be very difficult to confirm, especially among women (20).
In a 2004 study, larger waist size and high BMI have been associated with higher risk of colon cancer (21).
Waist sizes of 39 inch and higher showed a two-fold rise, and linearly increased thereon.
In the same study, BMI over 30 showed 50% higher risk of colon cancer in middle-aged (those below 55 years) and 2-and-half times higher risk in those over 55 years (21). Men were at higher risk than women. The reason behind this correlation is not clear. But factors under suspicion include higher calorie consumption, increased insulin resistance, and genetic or environmental factors.

Figure: The hockey-stick chart of health risk versus BMI. There is a substantially higher risk with increase in BMI over 25.
Fat distribution varies with age. For example, fat just below the skin declines but that around the internal organs increases with age (22).
The typical decline in BMI and waist circumference over age is mostly due to the decline in fat below the skin (besides the gradual decline in muscle mass with age).
This uneven distribution poses a challenge in understanding the role of BMI on heart health and cardiovascular disease. Body fat around the organs–called visceral fat–poses much higher risk of heart disease, especially for high cholesterol levels (22). The visceral fat is a common feature of middle age, with large fat gain around the belly.
The visceral fat plays a key role in helping thyroid maintain the body temperature.
An increase in BMI has several negative effects (23):
Hypertension is the most significant risk factor that shows a direct link to obesity thus increases risk of heart disease.
It lowers HDL–the good cholesterol–significantly.
Well known to causes high cholesterol levels (24).
Known to modestly raise levels of LDL–the bad cholesterol–and total cholesterol.
Strongly correlates to increase in blood pressure.
Responsible for raising blood sugar that builds insulin resistance and increases the risk of diabetes.
Proportionally lowers the LDL particle size (23)–which correlates to higher risk–independent of triglyceride levels which themselves are strong determiner of LDL particle size (25).
But does not correlate to Lipoprotein-A (LpA0 is an independent risk factor of heart disease as LpA is mostly determined by genetics (26).
Increases the risk of diabetes, especially in women (27, 14).
Shown to cause thickening of the walls of left chamber of heart, the portion responsible for pumping blood to the body (28).
Obesity was found to be a critical factor for atrial fibrillation (Afib, a disturbance in heart beat) increasing the risk by almost 50% (29).
Many other studies have highlighted the role of BMI on human health in different ways:
Higher BMI also shows correlation with certain types of cataracts (cloudy eyes that originate at the back surface of lens) (30).
Obesity has also been linked to spinal cord degeneration, increased risk of disc slippage with age (31) and arthritis of the knee (32).
BMI has also been shown to affect the bone mineral density (33).
The risks of weight gain and heart disease differ between men and women.
Women can gain weight almost throughout their life, although it stabilizes for men in their 50s.
Women tend to be more self-conscious of weight at almost any age, and normally have lower BMI compared to men (5).
But men are twice more likely to have heart disease (34). At the age of 40 years, risk of developing coronary heart disease during their life for men is 1 in 2, and for women 1 in 3 (35). At 70 years, it is 1 in 3 for men, and 1 in 4 in women.
A 1999 study suggests that 70% of the heart problems in obese women and 40% in overweight women are mainly due to weight gain and could be prevented by weight loss (36).
Early studies have reported that women’s risk of heart disease drastically increases after menopause. It rises rapidly, from 2 to 12 in every 1,000 cases. In comparison, the number is 25 in men at the age of 45 years (37). Women on hormone replacement therapy tend to have a higher risk of stroke (38). Higher BMI values in women strongly correlate to increased triglycerides, smaller LDL particle sizes, and diabetes–all risk factors for heart disease (5).
Almost 70% incidents of heart disease in women show chest pain (angina) vs only 30% in men. However, occurrence of sudden death in men is 4 times (20% versus 5%) in comparison to women.
Data suggest women have higher impact from hypertension but men are affected more from higher cholesterol (5).
There is no doubt that obesity increases risk of heart disease and has serious impact on health as shown by few examples from scientific research (39):
Obesity is a long term risk predictor of cardiovascular disease (CVD), especially among younger population, as it affects future health.
In women, it increases the risk of stroke independent of other risk factors; after age and blood-pressure, it is the third biggest predictor of cardiovascular disease in women.
At age 25, weight gain directly correlates to future risk of CVD. This correlation is stronger for men, based on a Framingham study that monitored 5,000 people over 26 years. This risk is even higher for those who had consistently higher weight over longer periods. That means, duration of obesity is also a risk factor for heart disease and has bigger impact on this risk. However, a long term monitoring is critical. Previous studies have shown that it took 8 years of follow-up for men, and 14 years for women to show a statistically significant impact.
Weight gain early in life was a good predictor of hypertension in women (but not in men), on 26 years of data.
Higher concentrations of fiberinogen–protein responsible for blood clotting–has been found with increased obesity (40).
In cases of high obesity, the workload for heart increases and enlargement of heart in size and weight has been observed (41).
Younger obese individuals, without any symptoms of heart problems, might already have a compromised heart on close inspection (42).
Surgeries of Framingham population after death has shown a increase in heart size with excess weight (43).
Monitoring weight is a crucial step for healthy heart. BMI is easy to calculate by measuring the weight and height.
Blood pressure measurements are common at a doctor’s office or at a nearby pharmacy. Walmart, Rite-aid, CVS, or local healthcare facilities have self-serving kiosks that allow measuring blood pressure. Small portable gadgets are available to purchase relatively inexpensively, for those regularly monitoring their blood pressure.
Other key risk factors of heart disease are easy to assess using a simple blood test. They can be part of your annual checkup, or you can order an at-home cholesterol and heart health test online. Simply collect sample at home using a finger prick and ship it back to the lab. The results are mailed to you within few days.
Depending on the type of test, the following markers are measured, with optimal values suggested by the Mayo Clinic (36):
Cholesterol – this is the total of all your cholesterol values – below 200 mg/dL is desirable.
HDL – high-density lipoprotein or the ‘good’ cholesterol – above 60 mg/dL is the healthiest.
LDL – low-density lipoprotein or the ‘bad’ cholesterol – below 70 mg/dL is the best.
Triglycerides – the fat in the blood – below 150 mg/dL is desirable.
A1c – the average of 90 days of red blood cells, also called HbA1c – below 5.7% or 154 mg/dL is normal (3).
hs-CRP – high sensitivity C-reactive protein is a newer marker for inflammation that has shown to be an excellent indicator of atherosclerosis and future cardiovascular disease (44). Values below 3mg/L are better.
Some tests also look at:
LDL particle size – some tests check for the size, smaller size is linked to higher risk (45).
Lipoprotein A – an independent marker of heart health (46), especially those with family history of heart disease (26).
Vitamin D – to ensure you have healthy levels, as low Vitamin D has been shown to impact cardiovascular health (47).
Using the Framingham 10-year risk score or a 30-year risk score, it is easy to calculate your risk of heart disease.
Weight gain, and corresponding risk of heart disease, are preventable with healthy life style and regular exercise. Reducing stress and sleeping for 6 to 8 hours also help in lowering and maintaining a healthier BMI. Watching the portion size, avoiding sugary and fatty foods, eating more vegetables and fruits regularly, and fasting intermittently are also popular methods for a healthy heart.
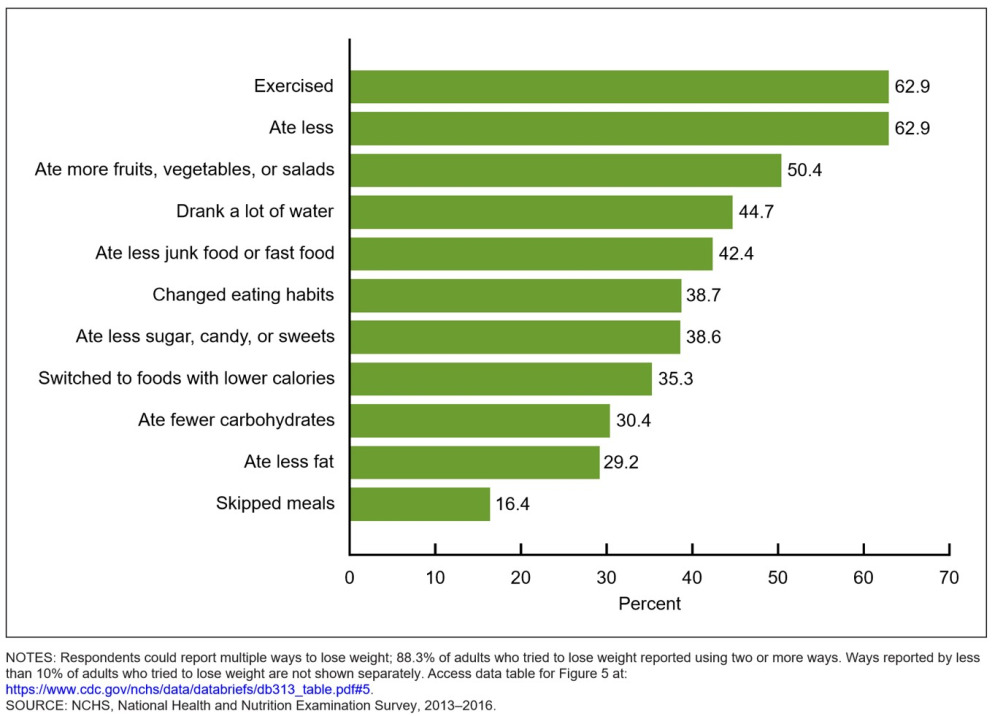
The CDC data from survey of US population show that the most common methods of loosing weight are exercise and eating controlled portions.
This article on the obesity as risk factor for heart disease is provided for information purposes only. Not for diagnosis or to replace advice from a medical professional. Our at-home Cholesterol and Heart Health Test, Inflammation and Vitamin D Test or a Pre-diabetic A1c Test can be ordered online. See the full list of CLIA-certified health tests at www.RxHomeTest.com. All tests include a physician’s prescription, free shipping, and physician approved reports. Also available: Comprehensive food sensitivity test, celiac genetic test, pre-Alzheimer’s APOE genetic test, at-home Thyroid test, Inflammation and Vitamin D test, Cholesterol and Heart Health Test, Pre-diabetic A1c Test, Gut health test and H. pylori test, cortisol saliva test, sleep and stress test, at-home metabolism test, women’s health test, men’s health test, at-home testosterone test, and many more health test options.