
This article covers: Cortisol stress hormone, Diurnal cortisol rhythm, Cushing’s syndrome, Addison’s syndrome, Cortisol stress test.
What is cortisol?
It is one of the stress hormones from adrenal glands. Essentially, a catabolic steroid hormone that helps in breaking down muscles and bones to store fat in the body.
Cortisol has a well-defined 24-hour circadian rhythm; levels rise quickly after waking up but then decline throughout the day.
Stress from everyday activities, such as public speaking or work related deadlines, can elevate cortisol levels to fight off the stress stimulants. That's why people with high stress also tend to have high cortisol levels.
Chronically high levels can cause fat accumulation—especially around the waist—and weak bones and muscles. Cortisol deficiency may result in fatigue, sluggishness, and no desire to exercise.
Using four saliva samples within 24 hours—in the morning, noon, evening, and night—it is possible to understand the diurnal rhythm of this stress hormone.
A flat trend, without morning peak, is strong indicator of Cushing’s syndrome, and possible issues with adrenal or pituitary glands.
In contrast, extremely low levels indicate Addison’s syndrome—a condition in which adrenal glands cannot produce enough cortisol (e.g., due to autoimmune disease).
By monitoring stress, exercising regularly, meditating, and eating healthy, one can maintain optimal cortisol levels.

Why Morning Cortisol Levels and Time are Important – levels fluctuate significantly after waking up.
How Can My Medicine Affect Cortisol Levels? - certain drugs tend to raise or lower normal cortisol levels.
Vitamin D and CVD – role of Vitamin D in heart health.
Thyroid and Your Health – how thyroid impacts each one of us.
About Healthy Metabolism - key markers for checking your metabolic health.
All About Testosterone and Aging – summary of research on the male hormone.
CRP and Heart Risk – read about a marker for low inflammation associated with heart attack.
Stomach Ulcers and H Pylori – learn about the Nobel Prize winning research on gut bacteria behind gastric ulcers.
Hormone Imbalance in Women – learn about the role of estrogen, progesterone and testosterone for women.
Ad-renal glands sit on top of kidneys and release the stress hormone hydrocortisone, also known as cortisol.
Cortisol helps in digesting glucose and belongs to an important group of steroid hormones called glucocorticoids (= glucose + cortex + steroid, i.e., steroid hormones produced in the adrenal cortex for glucose metabolism).
Glucocorticoid medicines are used in treating allergy, asthma, and autoimmune diseases to control an overactive immune system. Such catabolic steroid hormones break down tissues such as muscles and bones to accumulate fat.
Almost all the cells have a cortisol receptor, making it crucial for many different functions in the body. Although its most important role is in metabolism—by breaking down muscles, bones and building fat—it also helps regulate blood pressure, blood sugar levels, salt and water balance.
Cortisol is used in reducing inflammation and improving memory formation. During pregnancy, cortisol supports fetus development. There is a strong link between stress hormones and mood swings, which makes it an important hormone for overall health and well-being.
Corticosterone is a similar hormone, but only in birds, reptiles, and rodents.
Three different organs regulate cortisol levels. This so called HPA-axis includes hypothalamus and pituitary gland in the brain and the adrenal glands on kidneys.
Whenever cortisol levels are low, the hypothalamus releases a hormone called CRH (corticotrophin-releasing hormone), which directs the pituitary gland to release yet another hormone, ACTH (adrenocorticotropic hormone). The adrenal glands responds to ACTH in order to release cortisol. The hypothalamus monitors optimal levels to setup a closed loop feedback, with small tweaks in CRH values to maintain the desired levels .
In some ways, cortisol works like adrenaline—the hormone often associated with a sudden blast of energy. During stress, a temporary cortisol surge tries to fight off the stress: heart rate increases, breathing gets heavy, blood pressure and blood sugar rise, and muscles get tense. Digestion and reproduction shut down until the body can fight off this stress stimulant.
These short bouts help cope with the daily stress in life, however, chronically high levels accelerate the body's metabolism. As a consequence, an increase in appetite causes fat accumulation and weight gain—common observations in high-pressure jobs.
On the other hand, cortisol deficiency slows down the metabolism causing fatigue, sluggishness, weight loss, and no desire of physical work.
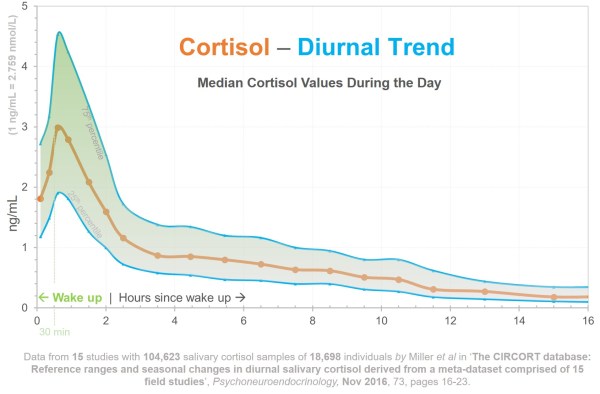
Figure 1: Diurnal (daily) cortisol trend, based on a summary of 15 different research studies (Miller 2016).
With a well defined 24-hour circadian rhythm, cortisol levels are highest in the morning after about 30 minutes of waking up. But then they continuously drop, reaching the lowest levels around 3 am. In a sense, this follows our daily energy levels, and are opposite of the sleep hormone, melatonin.
This cyclic pattern depends on sleeping habits, regardless of seasonal changes in sunrise or sunset. That's why night shift workers have different curves—the time for their peak depends on whenever they wake up.
Some studies suggest a small seasonal influence as well. An Australian study covering 13 years of data found about 5 percent change with every hour of later sunrise time (Figure 1). The peak levels were higher in winter with late sunrise (note that Australian is in southern hemisphere and it's winter in June and July).
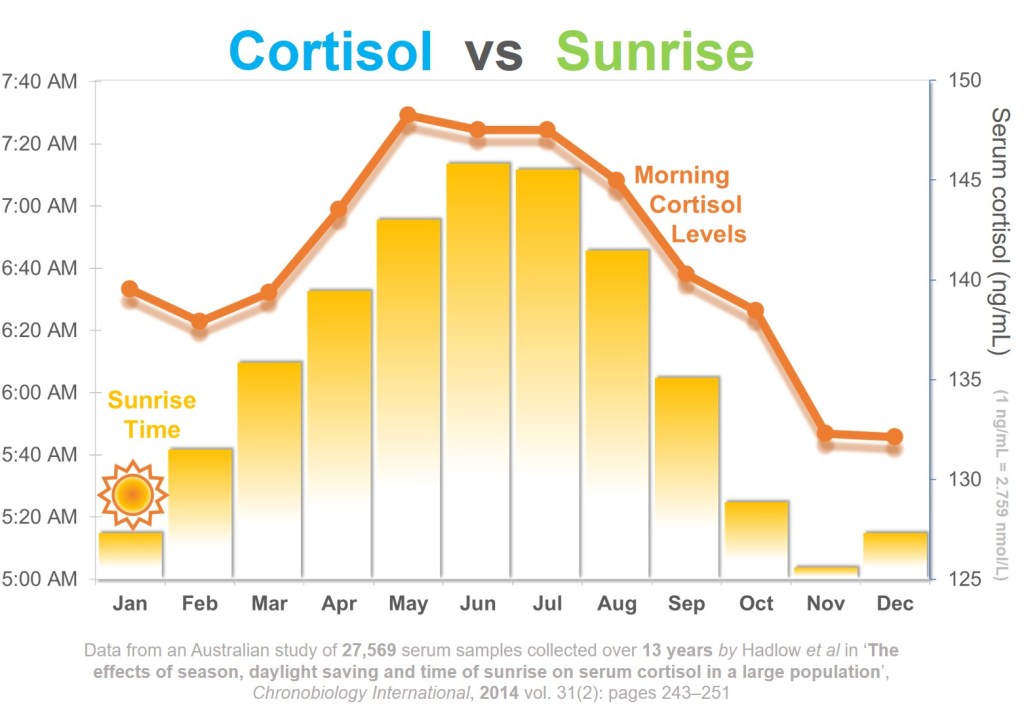
Figure 2: Change in morning peak levels with season and sunrise, from an Australian study conducted over 13 years (Hadlow 2013). Note that Australia is southern hemisphere and peak winter period is April to August.
Short bouts of high cortisol are good for the body to fight off any stress stimulants. However, chronically high levels have undesired consequences. The symptoms include:
Weight gain – high levels cause a build up of fat around the belly, chest, and face – a characteristic apple-like shape.
Increased appetite – cortisol stimulates hunger center in the brain, causing an unhealthy appetite.
Tissue breakdown – as a catabolic hormone—one which breaks down tissue, instead of building them—high levels result in fewer muscles and weaker bones with a slower than normal metabolism. That makes one feel weak and tired all the time. The breaking down of tissues, such as skin can cause easy bruising, stretch marks, and thinning of skin; breaking down of bone tissues can cause osteoporosis.
Immune suppression – stress hormone keeps the immune system in check by interacting with white blood cells and its anti-inflammatory properties. Excess levels can suppress the immune system and make us feel sick.
Upset stomach and ulcers – excess stress hormone cranks up acid production in stomach causing an upset stomach and potentially dangerous ulcers. People with chronically high stress are at higher risk of stomach ulcers.
Bloating and fluid retention – cortisol stimulates the hormone responsible for minerals and salt control in the body. In this role, it can increase retention of salt and water resulting in bloating. It can cause a drop in potassium levels, impeding insulin function and causing diabetes.
Changes in libido and menstrual cycles are also associated with high levels of cortisol.
Increase in thirst and frequent urination due to high appetite are potential symptoms of excess cortisol levels.
Cushing syndrome is an abnormally high production of cortisol, due to tumors in pituitary gland.
Although rare—affecting 1-in-1000 people—it disproportionately affects women, who are at four times higher risk than men.
Cushing has most of the symptoms associated with excess cortisol, as discussed above. Individuals with the syndrome show sudden gain in weight around their mid-torso, chest, abdomen, and face, often with thin legs and arms. Other symptoms include osteoporosis, high blood pressure, flushed round face, mood swings, and changes in the skin (e.g., bruises and stretch marks).
Addison's disease is a rare condition of insufficient cortisol, caused by an autoimmune disease of adrenal glands.
Symptoms of low cortisol levels are fatigue, loss of muscles, mood swings, and darkening of skin in different parts of the body. Also, dizziness when standing, weight loss, salt craving, low blood pressure often appear with Addison's disease.
Adrenal fatigue is a term applied to insufficient functioning of adrenal gland. Long term chronic stress can cause dysfunction of the glands, with symptoms that closely resemble Addison’s disease.
An adrenal stress test is a great way to assess the diurnal cortisol trend and check DHEA levels—a hormone precursor to several key hormones in the body.
Since cortisol has a well defined 24 hour circadian pattern, a 4-point cortisol test is one of the most popular tests. Four samples are collected throughout the day: morning, afternoon, evening, and night to understand the diurnal rhythm. For a basic understanding of your levels, an AM-PM test with one sample at the peak in morning and one in evening (or night) can be used. Tests can use saliva, urine, or blood samples.
Salivary cortisol testing is more popular than other methods. Checking cortisol levels using a salivary ELISA assay kit is a highly accurate and very reliable method. It offers several advantages over a blood test:
Stress-free sample collection, as often as necessary.
No lab or medical personnel necessary to collect the sample.
Saliva test measures free cortisol avoiding any aberrations in results from proteins that binds with it.
Lower cost due to the above reasons.
Avoids false positives from medication. The fraction of unbound free cortisol remains unchanged during medication, e.g., in women taking oral contraceptives.
The biggest hurdle to accuracy of salivary testing is the compliance with saliva sampling. In a controlled study collecting 6 samples over 24 hours, 25% of participants missed collecting their samples within a given window. However, a well communicated procedure can help avoid such problems.
The sudden rise in stress hormones due to external factors, such as fear, starts at a very early age.
Newborns and infants show such elevation due to stress. Among newborns, heel sticks, inoculation, or brief separation from mothers—all elevate stress hormones.
Other factors that determine how stress impacts the levels are:
Genetic differences: Studies on identical twins show similar cortisol response, before and after psychological stress, which suggests our responses are genetically programmed. However, no such behavior is seen with physical exercise. This suggests our health levels and the extent of psychological stress have very different response, outside of the genetic programming.
Sex difference: Men release 1.5 to 2 times more stress hormones than women on exposure to psychological stress. In controlled studies, although levels didn’t rise as high as in men, women showed larger decrease when they got short term social support from their partners.
Smoking: nicotine affects the HPA axis causing chronically high ACTH and cortisol levels. Smoking also raises stress hormones all day long. This can be problematic since smokers may respond less often to psychological stress when necessary, to fight the stress stimulus.
Physical exercise: cortisol levels start to rise during strenuous exercise, e.g., running a marathon. The levels peak 20-30 minutes after completion. However, low or moderate exercise may not show any rise. The effect of relaxation and meditation on reducing them is not yet fully understood.
Cutting down on stress – eating food is one of the most common ways of coping with stress. But it causes weight gain. The excess cortisol from stress triggers creates more fat, slows down metabolism, and breaks down muscles.
Eating small, frequent meals – they prevent surge in insulin and help to control hunger and cravings.
Cutting down on salt – salt causes bloating and high BP; it makes the body retain water and deprives the bones of calcium.
Reducing alcohol consumption – excess alcohol makes the adrenal glands overreact.
Quit smoking – nicotine affects the body’s ability to raise cortisol levels in response to any psychological stress to fight the stress stimulus.
Taking caffeine in moderation – caffeine raises the cortisol levels.
Physical activity is the best solution to lower stress and cortisol as it builds muscles, reduces fat in body, and improves insulin resistance; physical activity also takes the focus away from stress and the cravings to eat more.
Controlling hunger and focusing on other things prevent weight gain; it helps to avoid ‘comfort foods’ that have lot of fat & carbohydrates with high calories.
Improving self esteem and practicing positive self-talk help keep psychological triggers under control.
Meditation, Yoga, Thai-Chi, and Chi-Gong are known to lower stress.
Massage helps work the muscles and lower stress.
Making time for yourself by organizing and simplifying; working on your priorities helps with lower unexpected triggers of stress.
Spending time with family and friends prevents emotional triggers and motivates to follow our plans.
Being careful with herbal and medication products you use.

Order a 24-hour cortisol test kit.
Read ZRT lab’s excellent discussion and plots of diurnal cortisol curves for healthy individuals as well as patients with chronic stress, chronic fatigue, and burnout symptoms.
For the intricate details of a saliva based cortisol testing for Cushing Syndrome, learn from the experts at Mayo Clinic.
Cortisol vs pregnancy: The circadian rhythm of free cortisol in pregnant women starts to change around 20th week of pregnancy. Although the diurnal rhythm is maintained, the mean cortisol levels increase by 1.5-2 times with morning levels increasing several times higher than normal levels. Also, the peak levels lag behind approximately 90 minutes likely due to delayed activation of the HPA axis. The fact that external stimulation of CRH does not increase ACTH and salivary cortisol levels supports this observation. The levels return back to normal after 5-7 days of delivery. See the original publication: Psychoneuroendocronology, Vol. 19, No. 4, 1999 (page 317).
For information purposes only—not to be used for diagnosis or to replace advice from a medical professional. You can order multiple saliva hormone testing kits: a basic At Home Cortisol Test (for morning and evening samples) or a comprehensive diurnal cortisol test for checking the 24 hour circadian rhythm. Information on other health tests can be found here See the full list of CLIA-certified at-home health test from www.RxHomeTest.com for free shipping and physician-approved reports.