A thin mucous lining protects the stomach skin from food digesting acids. But damage to this protective lining causes ulcers that manifest as pain and burning sensation, whenever the acids contact the skin .
The food pipe, stomach, and duodenum—where the stomach joins the intestine—are most common areas of peptic ulcers.
Ulcers are difficult to diagnose. An endoscopy, which takes an image of the stomach, is the best way to diagnose and confirm the symptoms.
Historically, it was believed stress and lifestyle caused stomach ulcers. However, in 1980s, two Australian scientist discovered that Helicobacter pylori bacteria were the root cause of most stomach ulcers.
These bacteria can successfully survive the acidic environment by producing ammonia. Cancers from pathogens are extremely rare, but its role in gastric cancer as the second leading cancer worldwide is well established.
H. pylori is common: almost half of the global population harbors it without any symptoms. Better hygiene and low smoking rates have helped reduce the infection rates.

Figure: Better hygiene and smoking has dramatically reduced H. pylori infection. Data from Japan show a significant drop, from 68% to 5%, in people born within 75 years.
The widespread use of aspirin and NSAID medicines—nonsteroidal anti-inflammatory drugs for pain and fever purchased over-the-counter e.g., ibuprofen—has also contributed to ulcers. However, development of acid reducing medicines (PPIs, i.e., proton-pump-inhibitors, such as Nexium, Omeprazole) has been helpful in reducing the symptoms.
With regular use, the risk of ulcers increases four-fold from NSAID and two-fold from aspirin.
Not all causes of stomach ulcers are known. In fact, one in five cases occur in people without prior history for H. pylori or NSAID or aspirin. Certain events, e.g., spike in ulcers after 2011 earthquake in Japan or high prevalence in new refugees, suggest there maybe other causes that we do not yet fully understand.
Lack of clear symptoms makes it very difficult to determine the prevalence of stomach ulcers.
The most reliable data come from Sweden's 2001 Kalixanda study. Results of 1,001 endoscopies—in people with commonly known symptoms of pain, indigestion, heart burn, nausea, and vomiting—only 41 had ulcers. This amounts to a confirmed ulcer diagnosis of 1-in-25 people with known symptoms.
Moreover, 1-in-5 endoscopies with ulcers showed no symptoms. And, elderly patients rarely had any symptoms.
For every thousand doctor visits worldwide, only 1-2 are related to ulcers. Among those in the hospitals, the numbers are comparable (0.3 - 2 per 1,000).
During a lifetime, the risk of ulcer is about 5-10%.
There are two types of stomach ulcers based on their location:
Gastric ulcers - in the main stomach area.
Duodenal ulcers - in duodenum, the region where stomach connects to the intestine.
Duodenal ulcers are more common. A characteristic symptom is stomach pain that subsides after eating, but returns within few hours. Smoking, low-dose aspirin (below 160 mg), and H. pylori infection are the top causes of duodenal ulcers.
Gastric ulcers may not always show any symptoms, though smoking, aspirin, and obesity make them worse.
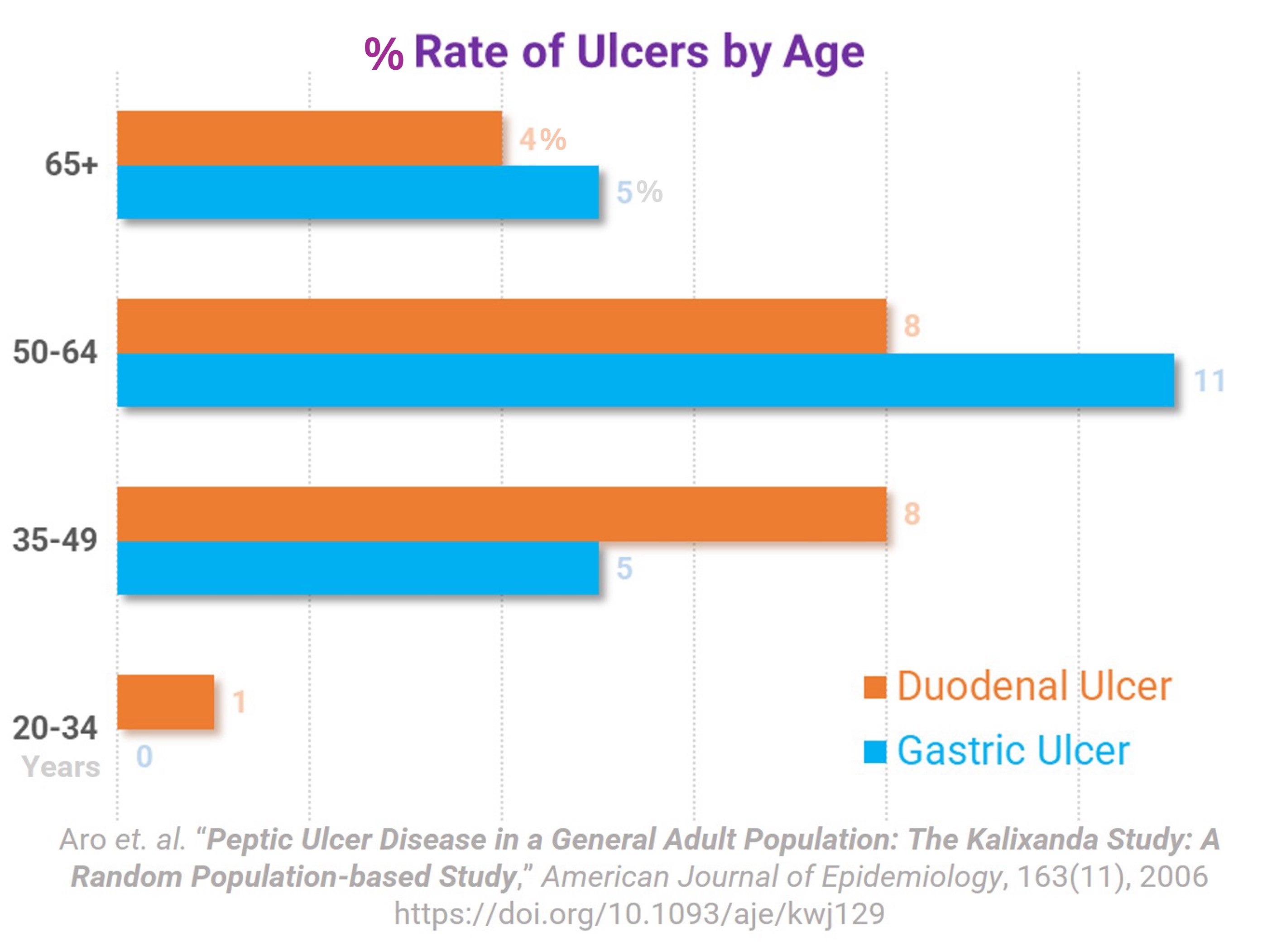
Plot from the Swedish Kalixanda Study above shows both ulcers occur at similar rates.
Symptoms of stomach ulcers overlap with other health conditions, which makes them difficult to diagnose without an endoscopy. However, following are commonly reported symptoms:
Stomach pain and discomfort
Acid reflux or heartburn (GERD)
Unexpected loss of weight
Blood in stool (or unusually dark, black color)
Indigestion (feeling full, bloating, gassiness, burning)
Vomiting, often with dark coffee color; or with sound of dry vomiting (retching)
In gastric ulcers, abdominal pain after a meal, nausea, vomiting and weight loss are more common. In contrast, symptoms of pain at night and feeling hungry often occur in duodenal ulcers.
In the Swedish Kalixanda Study of a thousand endoscopies, strongest indicators of ulcers was weight loss followed by nausea and heart burn.
More specifically, these symptoms—along with nausea, difficult swallowing, and retching (sound of dry vomiting)—were more common in gastric ulcers. On the other hand, urge to defecate at night was more frequently seen in duodenal ulcers.
Early detection of H. pylori is an effective way to avoid future ulcers. A stool test is recommended, however, a blood test for H. pylori allows testing for family members and larger groups.
Antibody test can detect past infections though a stool test is necessary to confirm current infection.
A triple therapy of antibiotics and PPIs is most effective treatment with almost 85% effectiveness. A bismuth based therapy maybe necessary during reinfection or for those with antibiotic resistance during first treatment. A second test is almost always necessary to confirm the full elimination of the bacterial.
Family members might need testing to avoid future reinfections.
Six-to-eight weeks of PPI normally heals the lining as acid control is crucial to the healing. However, in untreated peptic ulcers, symptoms frequently lapse due to simultaneous healing and relapse.
Although most treatments are successful, several challenges and complications may require further attention.
Complications include bleeding, perforation or blockage of the gastric path. Almost half of the complications include bleeding, which might happen without any signs. Perforation occurs with sudden intense pain on upper abdomen.
Fatality is highly dependent on age and secondary health conditions but they range in about 5-10% cases.
Several plant based herbal ingredients might also find use in certain cases. These include Korean red ginseng, green tea extract, garlic (allium sativum), laurel-leaf cistus (rock-rose), ginger. and turmeric. More data maybe required to confirm the effectiveness of these treatments.

H. pylori and Acidity - Key Facts - a comprehensive review of H. pylori.
Celiac – FAQs - key facts about gluten intolerance.
Sensitivity to Food – Allergy, Intolerance, and Celiac Disease - a comprehensive review.
What is Celiac? History, Present and Genetic Risk - A detailed look at celiac.
A Brief History of Gluten-free Diet - from banana diet to today's popular GF diets.